The Role of Simulation in Healthcare Decision Making
Healthcare is one of the information-heavy and high-stakes decision-making environments in the world. From doctors at the bedside diagnosing a sick patient under time pressure to hospital managers weighing policy options for an overwhelmed ICU during a pandemic the quality of
decisions made in healthcare directly determines patient outcomes, resource efficiency and institutional resilience.
Yet the science of healthcare decision-making, which includes how practitioners reason, how systems process evidence and how learners are trained remains under-discussed outside specialist circles.
How Clinical Reasoning Has Evolved
Decision-making in healthcare has changed from being individual and experience-based to a more structured and collaborative model. The increasing complexity in care along with the rapid expansion of scientific knowledge has made it necessary to integrate evidence, multidisciplinary expertise and contextual awareness into every layer of clinical practice.
Clinical decision-making (CDM) is the process by which healthcare professionals assess patients’ conditions and determine the care to provide. Traditional CDM is based on either intuition or conscious inference using well-defined logical frameworks applied in real-time. In practice both operate simultaneously in tension with each other.
Evidence-Informed Decision-Making (EIDM)
At the level this process is expressed in Evidence-Informed Decision-Making (EIDM), defined by the World Health Organization (WHO) as the use of the best available evidence to guide health policy and practice. The WHO framework emphasizes that decision-making should be grounded in an evidence base, including research findings, health data and contextual knowledge rather than habit or hierarchy alone.
Training Healthcare Professionals to Decide
One area noticeably absent from frameworks yet essential to any honest discussion of contemporary healthcare decision-making is the role of clinical simulation technology in producing decision-capable clinicians. The best institutional framework for evidence-based decision- making and the sophisticated analytical model will ultimately fail if the practitioners using them lack the clinical reasoning skills to interpret evidence recognize deteriorating patients and make timely interventions under pressure.
Clinical simulation provides learners with the opportunity to encounter scenarios in a controlled environment. A pedagogical approach that has gained significant traction across nursing, medicine and allied health education.
As Padilha, Machado, Ribeiro and Ramos (2018) demonstrated, virtual simulation in nursing education supports the development of reasoning and enhances learners’ engagement and sense of preparedness when entering real clinical settings.
Decision-making under time pressure in ambiguous situations is not a simple application of explicit rules. It involves:
- Perception and pattern recognition
- hypothesis generation and diagnosis
- Risk tolerance
- Capacity to revise one’s assessment as new information arrives.
These skills are difficult to teach through lectures or textbooks; they require deliberate repeated practice in conditions that simulate the emotional and informational texture of real clinical work.
The Impact of Virtual Patients and Physiological Engines
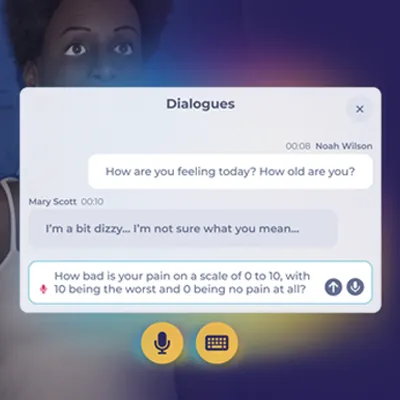
Virtual Patients such as Body Interact represent a step forward in this regard. Built on a real-time physiological engine Body Interact models each patient as a living system: vital signs shift in response to clinical actions organ systems compensate or deteriorate and the consequences of delayed or incorrect decisions unfold as they would in a genuine clinical encounter.
This kind of immersive consequence-driven learning environment aligns closely with what the cognitive science of reasoning tells us: that expertise is not merely accumulated knowledge but the ability to act on that knowledge under pressure with incomplete information and in real-time. A student who administers the wrong medication dose sees the patient’s condition deteriorate in accurate ways. A student who delays ordering an ECG in a suspected infarction experiences the time cost of that decision in a risk-free environment.
The reach of platforms has also been extended through remote and blended delivery. Ortiz-Arévalo et al. (2021) Showed that telesimulation and teledebriefing the application of simulation-based learning at a distance produce benefit in promoting clinical reasoning among undergraduate medical students offering an accessible model for institutions where in-person resources are limited.
Evidence From the Field: Clinical Validation
Comparative Trials in Medical Education
A pilot trial conducted at Universidad Andres Bello in Chile evaluated virtual patient simulation against small-group discussion for teaching myocardial infarction management to fourth-year medical students.
Students allocated to Patients showed improved OSCE scores and critically faster implementation of diagnostic and therapeutic interventions.
The ongoing integration of digital learning tools into healthcare professional education further
reinforces this direction. Padilha et al. (2021) Found that nursing students and practitioners
report levels of ease of use perceived usefulness and intention to engage with digital platforms when these are thoughtfully designed and contextually relevant. The barrier is not willingness; it is access and quality of design.
Closing the evidence-practice gap in healthcare is not only a question of better guidelines. It is also a question of how we develop the humans who must work within those systems and whether we give them the tools to practice reasoning before they face the consequences of getting it.
Simulation technology in its sophisticated forms is one of the most credible answers we currently have to that challenge.
Bring Evidence-Based Simulation to Your Institution
Align your training programs with global standards and the latest cognitive science in clinical reasoning. Discover why leading universities worldwide trust Body Interact to prepare the next generation of healthcare professionals.
References
Padilha, J. M., Machado, P. P., Ribeiro, A. L. & Ramos, J. L. (2018). Clinical Virtual Simulation in Nursing Education. Clinical Simulation in Nursing, 15, 13–18.
Ortiz-Arévalo, M. et al. (2021). Telesimulation and teledebriefing to promote clinical reasoning in undergraduate medicine students. Educacion Medica, 22, 283–286.
Padilha, J. M. et al. (2021). Easiness, usefulness and intention to use a MOOC in nursing. Nurse Education Today, 97.
World Health Organization. (2021). Evidence-informed policy-making: WHO guide. WHO.
https://www.who.int/publications/i/item/9789240039872
Author(s). (2023). Interprofessional clinical decision-making process in health: A scoping review. Journal of Advanced Nursing. https://doi.org/10.1111/jan.15865
Author(s). (2022). Clinical decision-making and nursing practice. PMC Article.
https://pmc.ncbi.nlm.nih.gov/articles/PMC8961960/
Martinez F T, Soto J, Valenzuela D, et al. (October 23, 2023) Virtual Clinical Simulation for Training Amongst Undergraduate Medical Students: A Pilot Randomised Trial (VIRTUE-Pilot). Cureus 15(10): e47527. doi:10.7759/cureus.47527